Thanks to advances in biomedical engineering, the use of robotic systems in surgery has become increasingly common. A clear challenge in robotic surgery, however, is the lack of haptic technology — there have been limitations in the ability to provide force feedback to the surgeon. Because many medical devices and surgical tools such as grippers and laparoscopic instruments do not provide tactile sensation, there has been no definitive way for a surgeon to sense how much force is being applied when using the instrument. This lack of tactile feedback limits the range of surgical techniques and affects the surgeon's dexterity.
Tekscan, South Boston, MA, a manufacturer of force sensors, has developed a sensor that is a key component in a noninvasive, haptic man-machine interface that provides tactile force feedback and ultimately advances the possibilities of what can be achieved with robotic surgery. The interface was developed by Cambridge Research and Development (CRD), Cambridge, MA.
Integrating the Sensors
CRD used Tekscan's FlexiForce™ tactile sensors in their research and development efforts on the haptic robotic interface to help improve robotic surgery by adding the sense of touch. FlexiForce sensors change resistance as force is applied, from megohms with no force to the low kilohms as force is applied. Conductance, the reciprocal of resistance, varies linearly with the applied force.
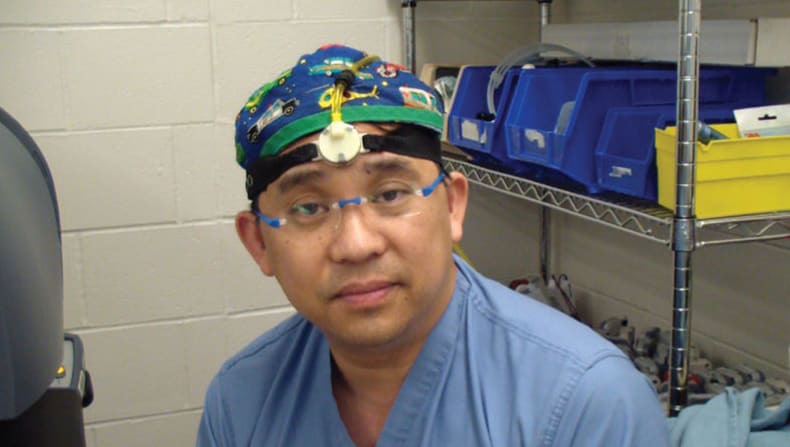
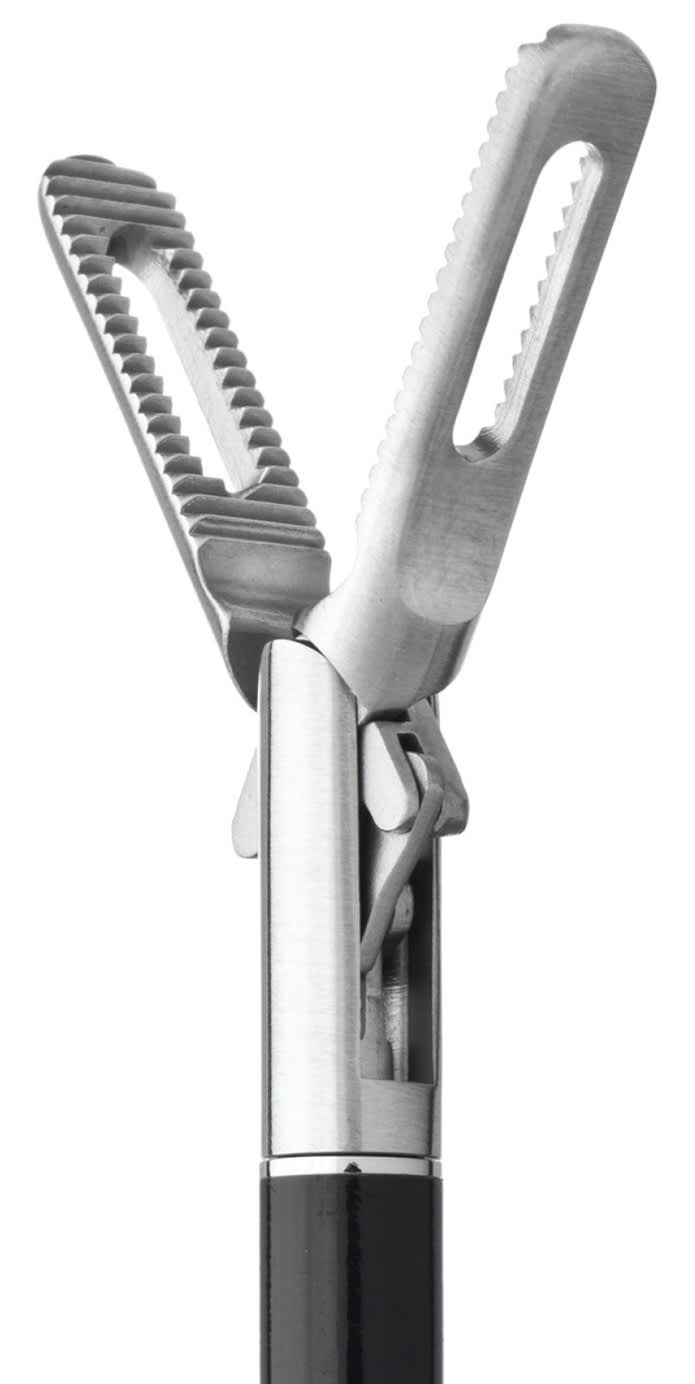
The interface that CRD developed, the Neo, uses linear actuation to provide force feedback. The mechanism mimics the sensation of force, through a device that can be worn anywhere on the surgeon's body, typically the head, in order to keep the surgeon's hands free. The very sensitive, thin (0.2 mm), and flexible FlexiForce sensor was placed in the front fenestration of a double fenestrated grasper. The fenestration is the part of the laparoscopic grasper that has a “window” in it, as shown in Figure 1. It is the contact point for the sensor, like a button that presses down on the sensor when tissue is squeezed. This sensor-enabled grasper is connected to the haptic interface. The FlexiForce sensor then measures applied force, which is translated into a pressure signal through the use of a mechanism that moves up and down in response to force. The brain associates the pressure applied by the device with a sense of touch, enabling the surgeon to respond by modulating their own applied force. For example, a surgeon wearing an apparatus on their head feels a tapping sensation that speeds up or slows down depending on the amount of force applied.The surgeon, seen in Figure 2, can learn to use it in about two minutes or less. The brain nearly immediately equates grasp with this pressure point.
An advantage of the integrated FlexiForce sensor is that it is so small and thin that it can easily fit into a compact device and still provide a full range of tactile sensation, from the initial lightest brush to a full grasp.
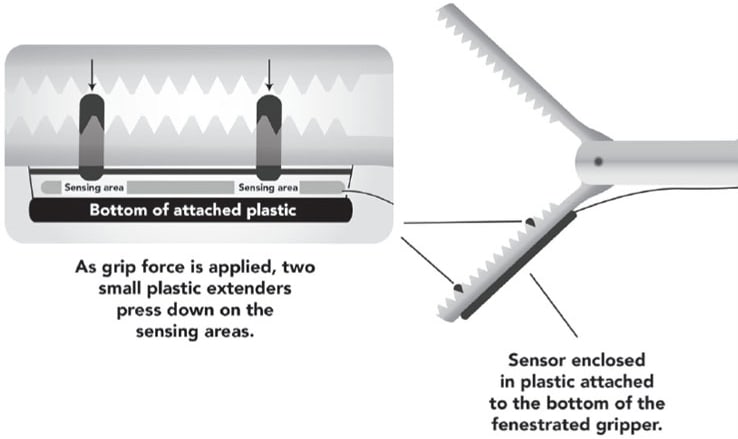
Since the sensor was embedded underneath the gripper, it was a challenge to design the setup so that the gripper load force could be transferred to the sensor. This was accomplished by using a small plastic mechanism, as illustrated in Figure 3.
Field-Testing the Interface
The FlexiForce sensor is lightweight, easy to integrate, and low-cost, which enabled CRD to demonstrate the potential for advancing robotic surgical tools and systems using tactile force feedback. Surgeons in the Department of Urology at Boston Children's Hospital, successfully simulated robotic surgical procedures using only the surgeon's sense of touch.
More intricate robotic surgical maneuvers have become possible thanks to the haptic feedback. Generally, a surgeon would not be inclined to grip a vein or delicate tissue with a laparoscopic surgical instrument for fear of damage. With a sensor-enabled device offering haptic feedback, the surgeon has much more control over the level of grip force applied. The same principle applies for movement of soft or lightweight objects during surgery.
The Future of Robotic Surgery
“The robotics industry understands that the true potential of robotics and cybernetics lies in the ability of man and machine to meld,” says Ken Steinberg, Cambridge Research & Development CEO. “Full bio-compatibility is in our future but advancements have to be made now if we are truly going to realize the potential of our robotic counterparts. With this new haptic interface, we feel we are providing a solution that will lead to new and exciting capabilities ranging from the surgery room to outer space.”
This article was written by Mark Lowe, VP Sensors, Tekscan (South Boston, MA), Ken Steinberg, CEO, Cambridge Research and Development, (Cambridge, MA), and Ed Brown, Associate Editor at Tech Briefs Media Group, (New York, NY). For more information, Click Here .

